Understanding Your Headache: A Real Guide to Finding Relief
Last Updated: April 2026
Let’s be honest—when your head is throbbing, the last thing you want is to dig through medical jargon. Whether it’s a dull ache after a long workday or a migraine that sends you to bed with the lights off, headaches are something most of us know too well. In fact, tension-type headaches alone affect between 46% and 78% of adults at some point in their lives
.
But not all headaches are created equal. Knowing what you’re dealing with is the first step toward feeling better. So grab a cup of tea (caffeine withdrawal is real, but more on that later), and let’s talk about what’s going on in your head—and what you can actually do about it.
The Big Three: Know Your Headache Type
1. Tension Headaches: The “Stress Band”
If you’ve ever felt like someone tightened a belt around your forehead, you’ve likely experienced a tension headache. These are the most common type, usually bringing a dull, constant ache on both sides of your head
.
What they feel like:
- Steady, pressing pain (not throbbing)
- Tightness in your neck and shoulders
- Sensitivity to light or sound, but usually no nausea
Common triggers:
- Stress (the obvious culprit)
- Poor posture (hello, laptop hunch)
- Skipped meals or dehydration
- Lack of sleep or, ironically, too much sleep
- Jaw clenching or teeth grinding
The human truth: These often sneak up on us during deadline week or after a night of poor sleep. Your body isn’t broken—it’s asking for a reset.
2. Migraines: More Than “Just a Bad Headache”
Migraines are neurological events, not just headaches. They affect about 12% of the population and are three times more common in women than men
. If you’ve ever had one, you know the difference.
What they feel like:
- Throbbing or pulsating pain, often on one side
- Nausea and vomiting
- Sensitivity to light, sound, and sometimes smells
- Worsening pain with movement
- Duration of 4 to 72 hours if untreated
The aura factor: About 25% of migraine sufferers experience “aura”—visual disturbances like zigzag lines, flashing lights, or blind spots that show up 5–60 minutes before the pain hits
. Note: If you experience these for the first time, seek medical attention immediately, as they can mimic stroke symptoms.
Common triggers:
- Hormonal changes (periods, pregnancy, menopause)
- Stress and anxiety
- Sleep disruption
- Certain foods (aged cheese, processed meats, red wine)
- Bright lights and loud noises
- Weather changes
3. Cluster Headaches: The “Alarm Clock” Pain
Cluster headaches are rare—only about 1 in 1,000 people get them—but they’re considered one of the most painful conditions a human can experience
. They tend to affect men more than women and often start in a person’s 30s or 40s.
What they feel like:
- Sudden, severe, piercing pain behind one eye
- Pain lasts 15 minutes to 3 hours
- Can occur up to 8 times per day
- Often happen at the same time daily, sometimes waking you from sleep
- Accompanied by a red, watery eye, nasal congestion, or drooping eyelid on the affected side
The human truth: People with cluster headaches often describe feeling restless and agitated during an attack—pacing the room rather than lying down. If this sounds familiar, please see a neurologist. You don’t have to endure this alone.
Headache Types at a Glance: Visual Comparison
Not sure which type you’re dealing with? This quick visual guide maps out where different headaches typically strike:
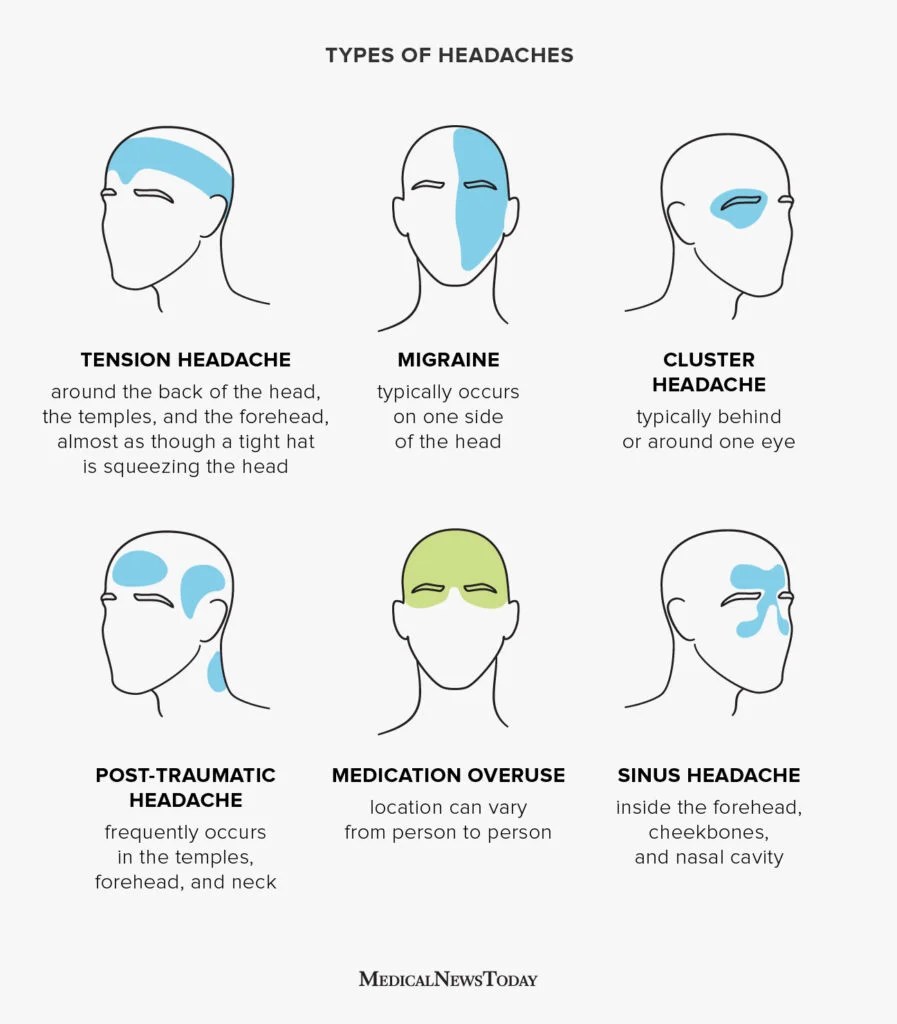
Here’s a more detailed breakdown comparing the big three side-by-side:

Other Headaches Worth Knowing About
Sinus headaches feel like pressure around your eyes, cheeks, and forehead, usually with congestion. However, research shows many self-diagnosed “sinus headaches” are actually migraines
.
Cervicogenic headaches originate from neck problems—muscle tension, arthritis, or nerve issues—and refer pain to the front of your head. Physical therapy is often the best treatment here
.
Exertional headaches strike after intense exercise, coughing, or even sex. They’re usually brief but can last up to two days
.
Medication-overuse headaches (rebound headaches) happen when pain relievers themselves become the problem. If you take headache meds more than 15 days a month, talk to your doctor
.
Thunderclap headaches are sudden, excruciating pains that peak within one minute. These are medical emergencies—call 911 immediately
.

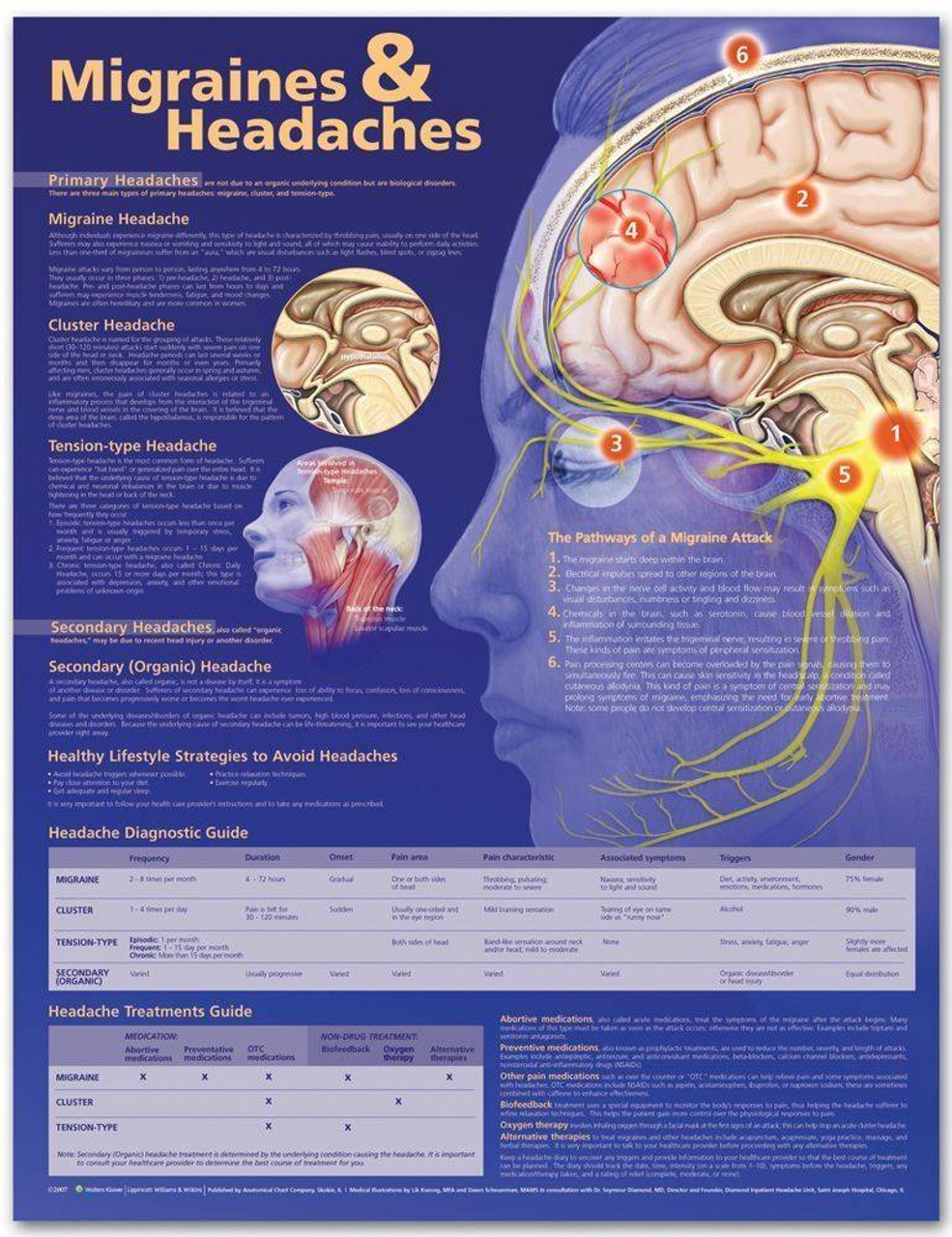
The Complete Headache Anatomy: What’s Happening Inside
Ever wonder what’s actually going on in your brain during a headache? This detailed mind map breaks down the different headache types by location, symptoms, and underlying causes:
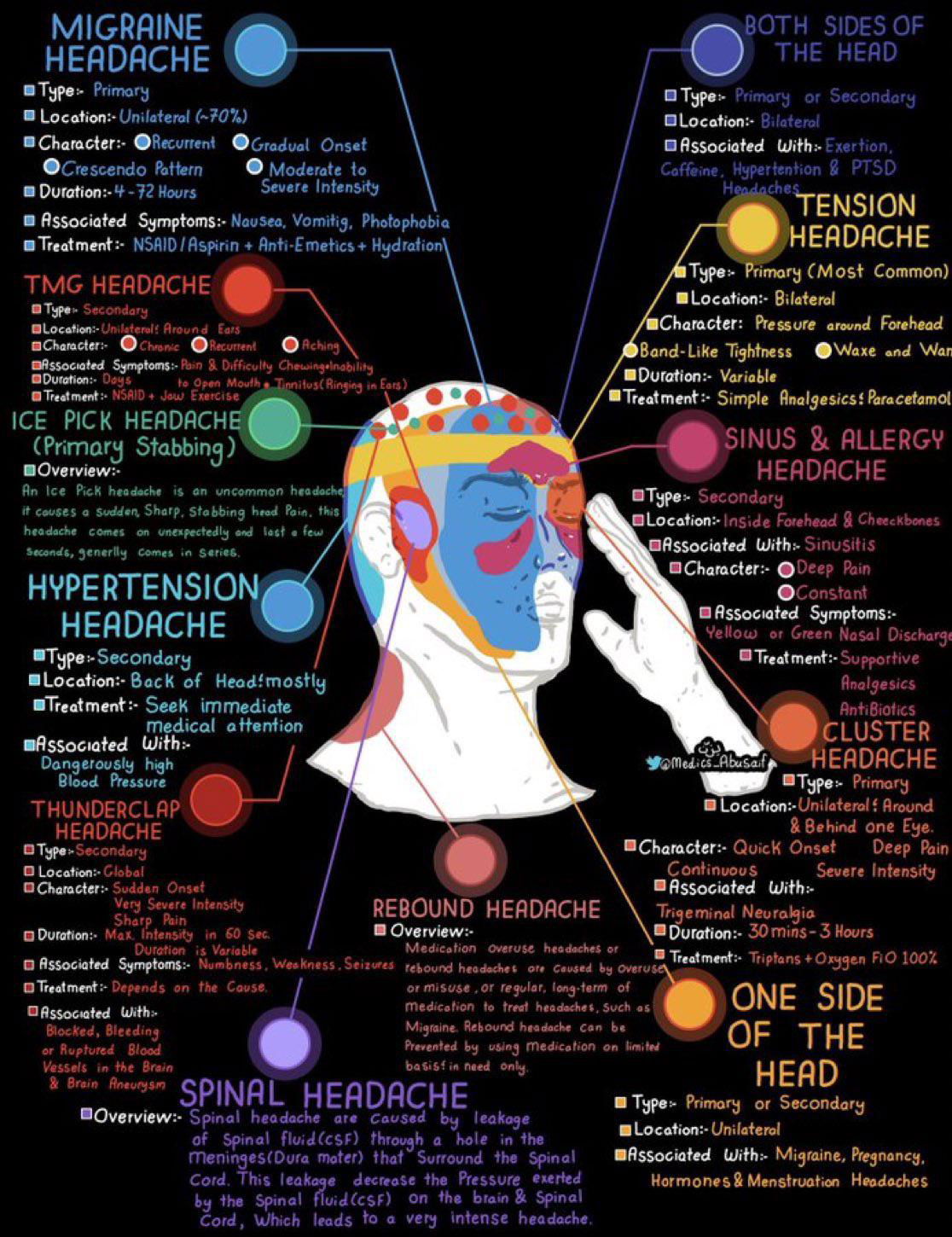
What You Can Do: Management That Actually Works
Immediate Relief Strategies
For tension headaches:
- A warm compress on your neck or a hot shower
- Over-the-counter pain relievers (ibuprofen, acetaminophen)
- Gentle neck stretches and shoulder rolls
- A quiet, dark room if light sensitivity kicks in
For migraines:
- Get to a dark, quiet room as soon as possible
- Cold compress on your forehead or neck
- Hydration—sip water or an electrolyte drink
- Prescription triptans if OTC meds don’t touch the pain
- Anti-nausea medication if needed

For cluster headaches:
- High-flow oxygen therapy (prescription)
- Triptans or prescription nasal sprays
- Verapamil for prevention during cluster periods
- Note: OTC painkillers usually don’t work for cluster headaches
The Headache Prevention Decision Tree
Not sure where to start? Follow this simple flowchart to identify your next steps:
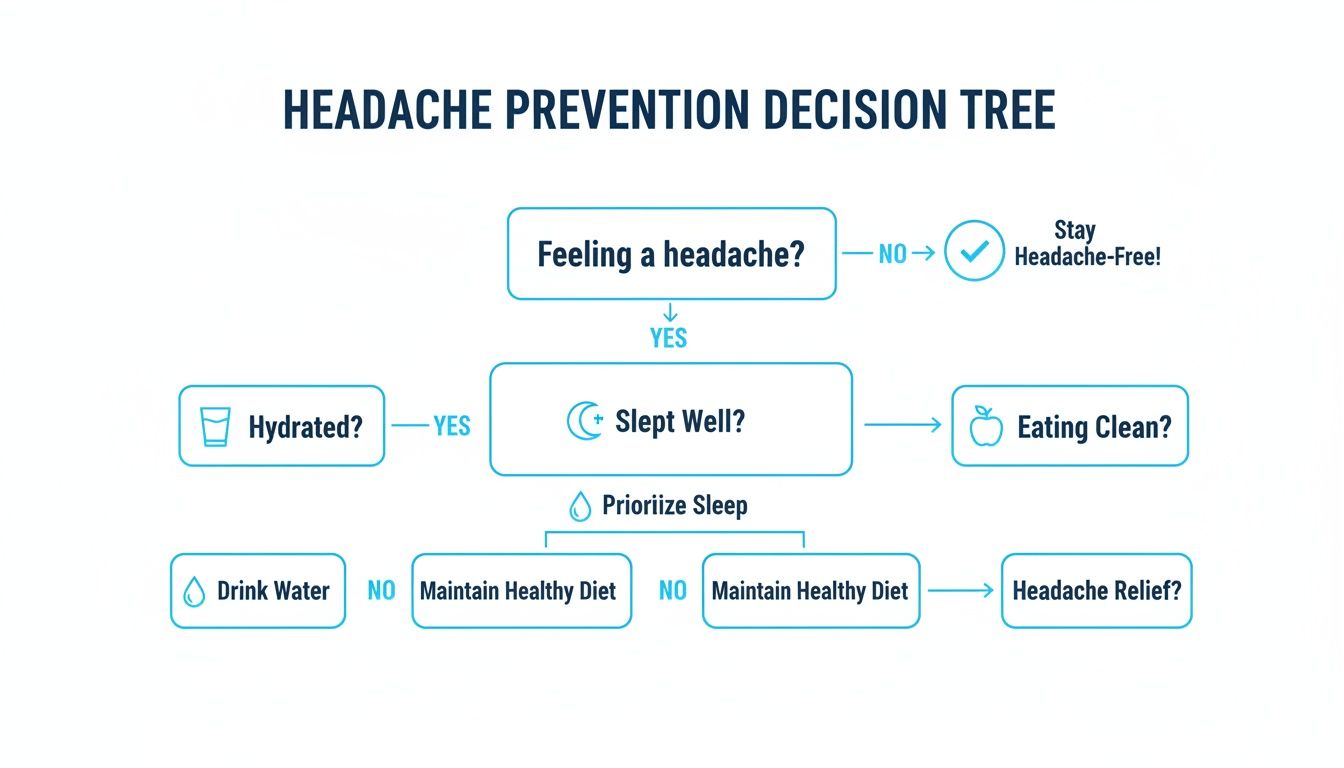
Long-Term Prevention: Building a Headache-Friendly Life
The best headache management happens between attacks. Here are evidence-backed habits that genuinely help:
Sleep like it matters (because it does) Aim for 7–9 hours of consistent sleep. Too little sleep triggers headaches; too much can too. Try to wake up at the same time daily—even on weekends
.

Hydration is non-negotiable Dehydration is a top trigger for tension headaches. Keep a water bottle nearby and aim for pale-yellow urine (yes, really—it’s the simplest hydration check)
.

Eat regularly Skipping meals drops your blood sugar and can invite a headache. Keep protein-rich snacks handy—nuts, yogurt, or hummus with veggies.
Know your food triggers For migraine sufferers, certain foods are notorious culprits. This trigger wheel shows the most common dietary offenders:
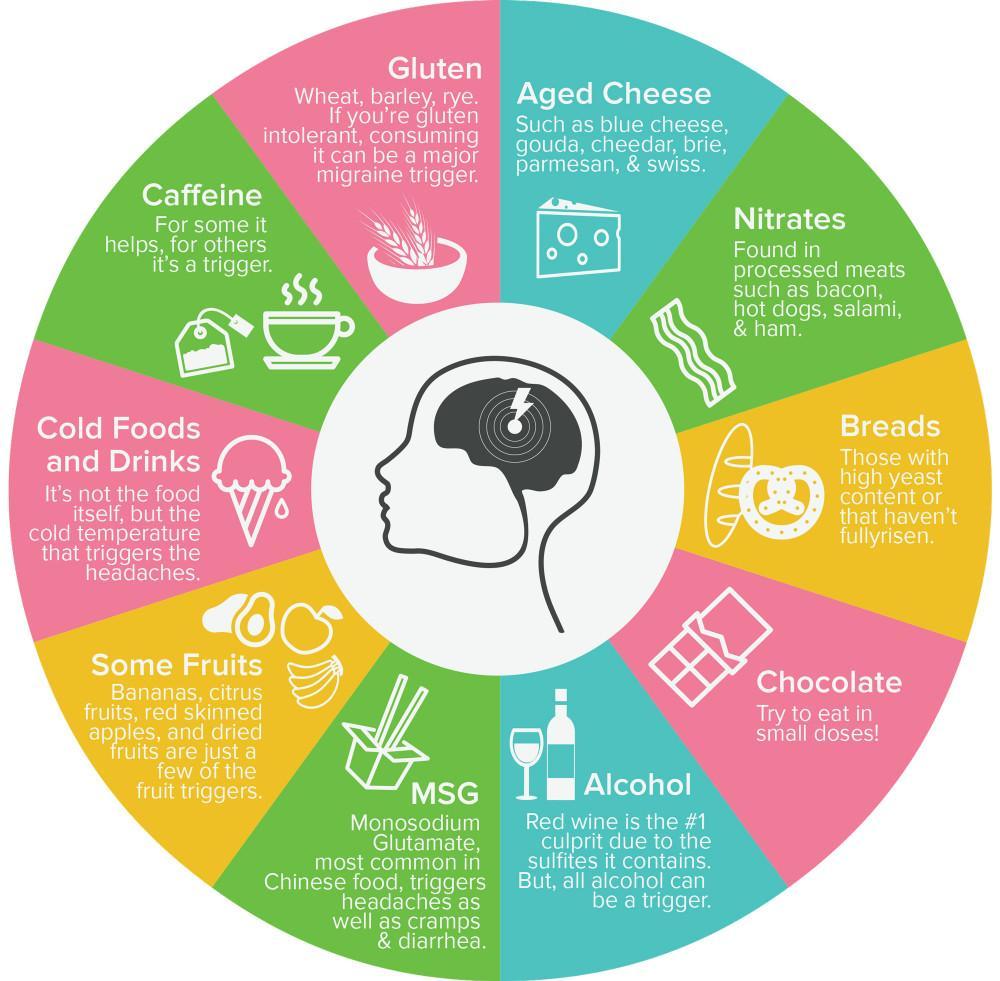
Move your body Regular exercise (30 minutes of heart-elevating activity, 3 times a week) reduces both the frequency and severity of headaches
. Start gentle if you’re headache-prone—sudden intense exercise can trigger exertional headaches.

Manage the stress Biofeedback, meditation, CBT, and even simple breathing exercises have solid evidence for headache prevention
. You don’t need to become a monk—just 10 minutes of deep breathing or progressive muscle relaxation can retrain your nervous system.

Watch the weather Barometric pressure drops, high humidity, and temperature swings can trigger migraines in sensitive people. If you’re weather-sensitive, tracking local pressure changes can help you prepare
.
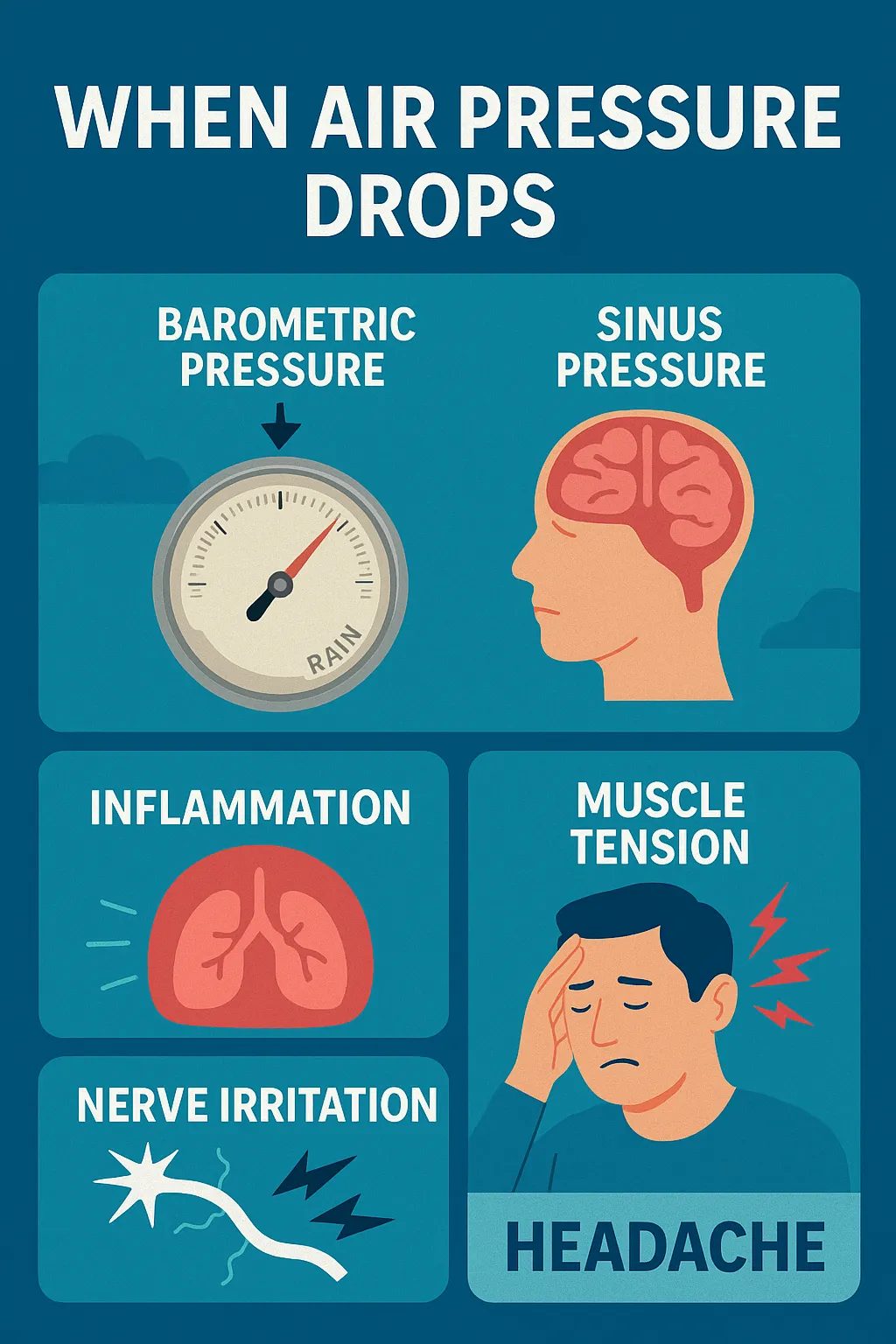
Living Well with Migraine: Behavioral & Lifestyle Guide
Migraine management isn’t just about pills—it’s about understanding the behavioral factors that contribute to your attacks and building a lifestyle that supports your brain:

Track Your Triggers: The Headache Diary
Knowledge is power, and patterns emerge when you track them. Use this simple diary template to log your headaches and identify your personal triggers:

Or try this more detailed visual tracker that maps pain location and severity:

Know Your Symptoms: The Headache Checklist
Not sure if it’s a migraine or something else? This symptom checklist helps you communicate clearly with your healthcare provider:

Migraine Facts & Figures: By the Numbers
Sometimes it helps to know you’re not alone. Here are the stark statistics about how headaches impact our world:

When to See a Doctor (Please Don’t Ignore These)
Most headaches are annoying but benign. However, seek immediate medical care if you experience:
- A sudden, severe “thunderclap” headache (peaks within 1 minute)
- Headache after a head injury, especially with confusion, vomiting, or memory loss
- Headache with fever, stiff neck, or rash
- Vision loss, double vision, or severe dizziness
- Weakness, numbness, or difficulty speaking
- A new or changing headache pattern, especially if you’re over 50
- Headaches that worsen with coughing, bending, or exertion
If your headaches are frequent (more than 15 days a month), increasingly severe, or interfering with work and relationships, make an appointment with your primary care doctor or a neurologist. There are preventive medications—like beta-blockers, CGRP inhibitors, and anticonvulsants—that can dramatically reduce how often you suffer
.

A Final Thought
Headaches aren’t a character flaw or something you should just “push through.” They’re your body’s way of signaling that something needs attention—whether that’s more water, less stress, better sleep, or medical treatment.
You deserve to feel good. Be patient with yourself as you learn your triggers and find what works for your unique body. Relief is possible, and you don’t have to figure it out alone.
Have a headache management tip that works for you? Share it in the comments—your experience might be exactly what someone else needs to hear today.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a healthcare professional for personal medical concerns.

